Anti-Fibrotic Properties
Keloids represent a challenging clinical condition characterized by excessive collagen deposition and persistent fibroblast activation, leading to raised, firm scars that extend beyond the original wound boundaries. Traditional treatments often yield suboptimal results with high recurrence rates. Emerging evidence suggests that amniotic membrane (AM) allografts, possess properties that can modulate fibrotic responses, offering a promising avenue for keloid management.
Shared Fibrotic Pathways in Corneal and Dermal Fibroblasts
Both corneal fibroblasts (keratocytes) and dermal fibroblasts involved in keloid formation share common fibrotic pathways, notably the TGF-β signaling cascade. In the cornea, AM has been shown to suppress TGF-β isoforms and their receptors, inhibiting myofibroblast differentiation and reducing scarring. Similarly, in dermal tissues, AM's anti-fibrotic effects have been observed, suggesting a potential crossover in therapeutic applications.
Keloid Revision
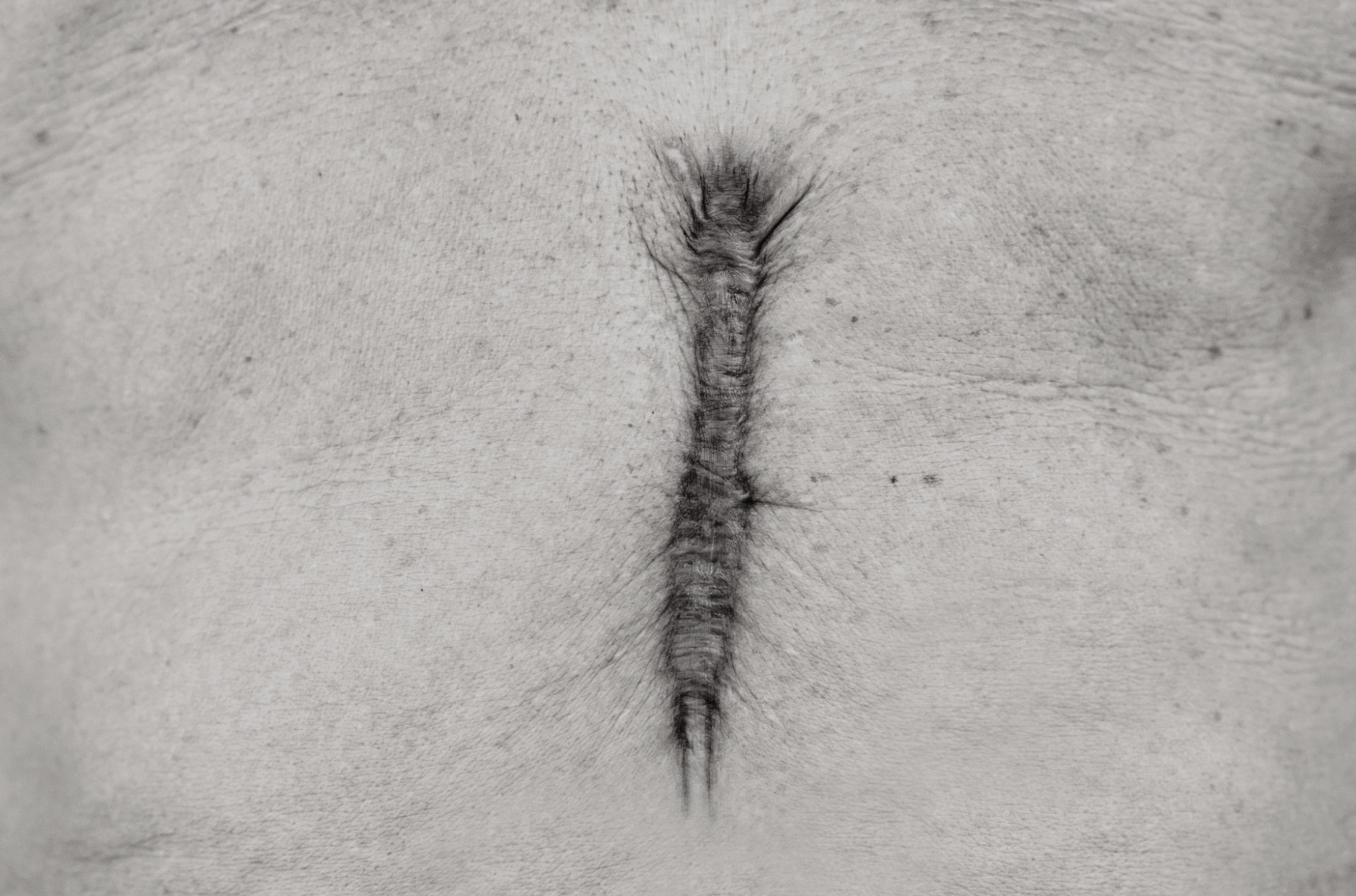
The anti-fibrotic and anti-inflammatory properties of amniotic membrane allografts support keloid revision, particularly for high-demand procedures like breast augmentation and cesarean scar management.
Mechanisms of Action
1. TGF-β Modulation: AM contains factors that downregulate TGF-β signaling, a key driver in fibrotic processes. By inhibiting this pathway, AM reduces fibroblast proliferation and collagen synthesis.
2. Anti-Inflammatory Properties: The AM matrix harbors anti-inflammatory cytokines that mitigate local inflammation, a contributor to keloid pathogenesis.
3. Extracellular Matrix Remodeling: AM promotes balanced collagen and proteoglycan synthesis, aiding in the restoration of normal tissue architecture and preventing excessive scar formation.
Clinical Implications
The application of AM in ocular surgeries has demonstrated its efficacy in reducing scarring and promoting regenerative healing. Translating these findings to dermatological contexts, particularly in the management of keloids, is supported by the shared fibrotic mechanisms. Preliminary studies have shown that application of AM post-keloid excision can lead to improved healing outcomes and reduced recurrence rates.
Conclusion
The anti-fibrotic and anti-inflammatory properties of amniotic membrane allografts, present a compelling case for their use in keloid management. By targeting the underlying fibrotic pathways common to both corneal and dermal fibroblasts, amniotic membrane allografts offer a biologically active solution to a condition often resistant to conventional therapies.
Start a Conversation

Clinical Considerations
Note: Graft sizes referenced are based on published clinical use cases and manufacturer specifications. Selection may vary by surgical technique, wound geometry, and provider preference. Always consult current literature and product instructions for use (IFU) for guidance.
1. Tseng, S. C. G., Li, D. Q., & Ma, X. (1999). Suppression of transforming growth factor-beta isoforms, TGF-beta receptor type II, and myofibroblast differentiation in cultured human corneal and limbal fibroblasts by amniotic membrane matrix. Journal of Cellular Physiology, 179(3), 325–
2. Eslahi, N., Nejad, Z. M., Rezaei-Tavirani, M., & Akbari, S. (2025). Amniotic membrane transplantation for wound healing, tissue engineering, and regenerative medicine. Stem Cell Reviews and Reports, 21(2), 345–359. https://doi.org/10.1007/s12015-025-10892-x
3. Bhatti, M., Adwan, A., Kamal, R., Singh, K., & Anand, S. (2024). Human amniotic membrane modulates collagen production and enhances wound healing. Scientific Reports, 14(1), 2789. https://doi.org/10.1038/s41598-024-64364-2
4. Davenport, B., Tatro, E., Phillips, H., & Yamin, F. (2019). Amniotic and umbilical cord particulate in the management of keloid and hypertrophic scars. Journal of Wound Care, 28(7), 456–462. https://doi.org/10.12968/jowc.2019.28.7.456A nice paragraph